MSGM Clinical Case Discussion April 2026
- Manali Patil
- Mar 31
- 3 min read
Balancing Acute Complications and Chronic Care: The Challenges of Optimizing Perioperative Management for Older Patients with Multiple Comorbidities
Prepared by: Dr Jeannie Phang Yik Tien
Supervised by: Dr Elizabeth Chong Gar Mit
Madam SA, a 72yearold Indian lady with multiple comorbidities and a Clinical Frailty Score (CFS) of 4, presented to the emergency department with right hip pain following a fall on a slippery floor. She sustained a right neck of femur fracture.
Comorbidities:
1. Bronchial asthma
2. Hypertension
3. Non-ischemic dilated cardiomyopathy with HFrEF
history of short run VT, dual-chamber implantable cardioverter-defibrillator inserted in 2015
-Coronary angiogram (Feb 2025): normal coronary arteries
-Echocardiogram (Nov 2024): EF 24%, global hypokinesia of the left ventricle
Home medications:
MDI budesonide 2 puffs BD
MDI salbutamol 2 puffs PRN
Empagliflozin 10mg OD
Atorvastatin 20mg ON
Cardiprin 100mg OD
Spironolactone 12.5mg OD
Entresto 25mg BD
Premorbid condition:
Clinical Frailty Score: 4
NYHA Class II
Mobility: ambulating unaided
Falls: no recent falls prior to current admission
bADL: independent
iADL: independent, able to cook, perform household chores, manage finances and medications
Cognition: intact
Sensory impairment: uses reading glasses, no hearing impairment
Social history: housewife, married with three children, lives with husband and youngest
daughter in a two room flat, without an attached bathroom.
Physical examination:
Oriented to time/ place/ person, coherent
No fever
BP: 128/70 mmHg
HR: 72/min
RR: 18/min
Spo2: 99% on room air
Respiratory: clear breath sounds
Cardiovascular: no murmur
Abdomen: soft and non-tender
Lower limbs: Tenderness over the right hip, no pedal oedema, calf soft and non-tender
Investigations:

ECG: Paced rhythm
Chest X-ray: Cardiomegaly
Pelvis X-ray: Right neck of femur fracture


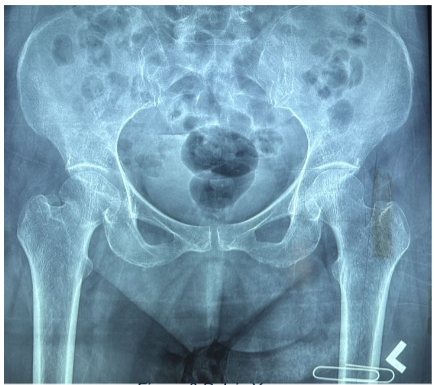
Hospital Course:
Day 1–3 Input/Output Charting:
Day 1: 660/900 → negative balance 240 mL
Day 2: 700/1200 → negative balance 500 mL
Day 3: 1000/900 → positive balance 100 mL
Day 2: Reviewed by geriatric, anaesthesiology, and orthopaedic joint replacement teams during Fracture Liaison Service (FLS) round. Empagliflozin was withheld, though the morning dose had already been administered.
Day 4: Madam SA began fasting after breakfast at 8:00 a.m. with two pints of normal saline infusion. She subsequently underwent right bipolar hemiarthroplasty under combined spinal‑epidural anaesthesia at 6:35 p.m., with the procedure lasting two hours.
Intraoperative:
BP: 100–125/58–68 mmHg
HR: 92–95/min
SpO₂: 97–98% on nasal prongs at 3 L/min
Estimated blood loss: 300 mL
Fluids: 1 L normal saline intraoperatively, continued with IV normal saline at
40 mL/hour
Postoperative:
Admitted to PACU for close monitoring.
Two hours postoperation: developed hypotension (BP 88/60 mmHg).
Eight hours postoperation: developed euglycemic diabetic ketoacidosis.
o IV fluids increased to 60 mL/hour.
o Started on insulin fixed scale and noradrenaline infusion at 0.2 mcg/kg/min.
o Euglycemic ketoacidosis resolved within 6 hours.
IV fluids reduced to 40 mL/hour and noradrenaline successfully weaned off.
Transferred back to orthopaedic ward acute bed.

Day 7: Patient recovered well, able to ambulate with a walking frame. Entresto, spironolactone, and empagliflozin were not restarted at discharge due to borderline lowish blood pressure (100–115/68–72 mmHg). An early followup appointment was arranged to review blood pressure and reinitiate her heart failure medications.
Discussions Part A:
1.How long should SGLT2 inhibitors or GLP-1 receptor agonists be withheld prior to major surgery to reduce the risk of perioperative complications?
2.Should hip fracture surgery be delayed to allow an optimal washout period of SGLT2 inhibitors or GLP-1 receptor agonists, or does the morbidity of delaying fixation outweigh the risk?
Discussions Part B:
1.How do we balance the risks of withholding heart failure therapy against the risks of hypotension and peri-operative instability?
2.Are the 4 pillars always indicated in elderly population with heart failure as per
recommendation?
3.In elderly post-operative patients, how should clinicians prioritize which heart failure medications to initiate first?
References:
1. American College of Cardiology. Preoperative Cessation of SGLT2 Inhibitors. Published October 7, 2022.
2. American Society of Anaesthesiologists. Consensus-based guidance on preoperative management of patients on GLP-1 receptor agonists. Published June 2023.
3. Tammy L. Kindel, Andrew Y. Wang, Anupama Wadhwa, Allison R. Schulman, Reem Z. Sharaiha, Matthew Kroh, Omar M. Ghanem, Shauna Levy, Girish P. Joshi, Teresa L. LaMasters, Multisociety clinical practice guidance for the safe use of glucagon-like peptide-1 receptor agonists in the perioperative period, Surgery for Obesity and Related Diseases, Volume 20, Issue 12, 2024, Pages 1183-1186.
4. Lam C, Thiruvenkatarajan V, Nanjappa N, Endlich Y, Lin D-Y. Perioperative management of glucagon-like peptide-1 receptor agonists: international guidance and variability in recommendations. British Journal of Anaesthesia. Published Feb 2026.
5. Davide Stolfo, Gianfranco Sinagra, Gianluigi Savarese , Evidence-based Therapy in Older Patients with Heart Failure with Reduced Ejection Fraction, Cardiac Failure Review 2022;8:e16.
6. 2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines.
7. Malaysian CPG Management of Heart Failure 2023.

Comments